Understanding Pancreatic Cancer: Key Facts and What to Avoid
Learn essential information about pancreatic cancer, including symptoms, diagnosis, treatments, and dietary guidance. Discover which foods pancreatic cancer patients should avoid and how lifestyle choices can support treatment and recovery.Pancreatic cancer develops in the tissues of the pancreas, an organ located behind the lower part of the stomach that plays a vital role in digestion and blood sugar regulation. This type of cancer can be challenging to detect early, as symptoms often do not appear until the disease is advanced. Knowing what to look for and understanding the condition is critical for improving outcomes and making informed decisions about treatment and care.
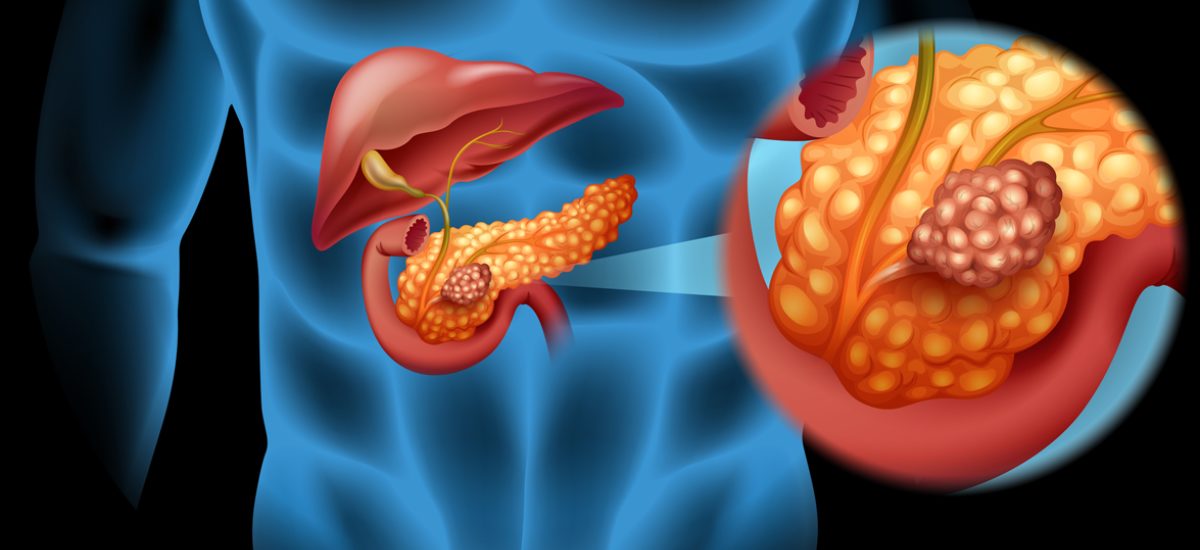
arly Signs and Symptoms
Symptoms of pancreatic cancer vary depending on the stage and location of the tumor. Common signs include abdominal pain radiating to the back, jaundice (a yellowing of the skin or eyes), unexplained weight loss, loss of appetite, nausea, and changes in stool color or consistency. As these symptoms can resemble other digestive or metabolic conditions, it is vital to consult a healthcare provider for proper evaluation if they occur or persist.
According to the National Cancer Institute, individuals with certain risk factors should be particularly vigilant. These include a family history of the disease, chronic pancreatitis, diabetes, obesity, or exposure to tobacco. Genetic testing and regular screening may be appropriate for those with inherited cancer syndromes such as BRCA mutations or Lynch syndrome.
Diagnosis and Medical Evaluation
Diagnosing pancreatic cancer typically involves imaging tests, blood tests, and sometimes tissue biopsies. Common diagnostic tools include CT scans, MRI, and endoscopic ultrasound, which allow physicians to visualize the pancreas in detail. The tumor marker CA 19-9 is often measured in the blood to help track disease progression and response to treatment, although it is not used for routine screening due to limited specificity.
Physicians may also use techniques like endoscopic retrograde cholangiopancreatography (ERCP) to examine bile ducts and ducts within the pancreas. Accurate staging determines whether the cancer is resectable (surgically removable) or has spread to nearby tissues or distant organs. This information guides treatment planning and helps predict long-term outcomes.
Treatment Options and Innovations
Treatment for pancreatic cancer depends on the stage and health of the patient. For early-stage disease, surgical removal of the tumor offers the best chance for long-term survival. The Whipple procedure, or pancreaticoduodenectomy, is the most common surgery, often followed by chemotherapy or radiation to eliminate any remaining cancer cells.
For advanced cases, palliative care focuses on extending life, managing pain, and improving quality of life. Recent advances in immunotherapy, targeted drug therapies, and genetic profiling have expanded the range of available treatments and increased hope for patients with previously untreatable forms of the disease. To explore new treatment trials, patients can visit the U.S. Clinical Trials Registry for information about current studies.
Comprehensive cancer centers often provide multidisciplinary teams that include oncologists, gastroenterologists, nutritionists, and mental health specialists. These teams help patients navigate complex treatment decisions and provide holistic care throughout the recovery process.
Nutrition and Foods to Avoid
Diet plays an important role in managing pancreatic cancer symptoms and supporting overall health during treatment. Because the pancreas contributes to digestion, patients may experience difficulty breaking down fats, leading to malabsorption, bloating, or diarrhea. A registered dietitian can customize a dietary plan that minimizes discomfort and helps maintain body weight and strength.
Pancreatic cancer patients should avoid foods that are difficult to digest or that can worsen inflammation. Key examples include:
-
Fried and high-fat foods like french fries, bacon, and burgers.
-
Processed meats such as sausages, hot dogs, and deli meats high in preservatives.
-
Sugary pastries and refined carbohydrates that may cause blood sugar spikes.
-
Alcohol, which can irritate the pancreas and interfere with treatment.
-
Heavy creams, cheeses, and butter that may be poorly tolerated without enzyme replacement therapy.
Instead, patients should focus on lean proteins (such as fish and poultry), whole grains, fresh fruits and vegetables, and plant-based fats like olive oil and avocado. Hydration is crucial; small, frequent meals are often easier to tolerate than large portions. Enzyme supplements may be prescribed to help the body absorb nutrients more efficiently, alleviating digestive strain.
Supporting Treatment and Recovery
Complications from pancreatic cancer, such as weight loss or fatigue, can be managed with a combination of medical support and lifestyle adjustments. Incorporating gentle physical activity as tolerated can help maintain muscle mass and improve mood. Support groups, both in-person and online, provide emotional comfort and practical advice from others facing similar challenges.
The American Cancer Society offers comprehensive guidance on managing side effects, finding treatment centers, and accessing financial or counseling support. Patients and caregivers alike benefit from connecting with social workers or oncology nurses who help coordinate care and offer reliable resources.
What You Should Know About Prognosis
Pancreatic cancer remains one of the most serious cancer diagnoses, but early detection and modern treatments continue to improve outcomes. Five-year survival rates vary widely depending on stage at diagnosis, overall health, and treatment accessibility. People with localized or surgically resectable tumors have significantly better chances of long-term remission than those with advanced disease.
Ongoing research efforts are accelerating discoveries in early detection biomarkers, improved imaging methods, and new medications designed to target specific cancer mutations. Supporting this research and participating in clinical studies can contribute to future progress in fighting pancreatic cancer.
When to Seek Medical Help
Anyone experiencing persistent digestive discomfort, unexplained jaundice, or sudden weight changes should consult a doctor promptly. Early testing, even if symptoms seem minor, allows healthcare professionals to address possible pancreatic disorders before they progress. For information about cancer care guidelines, visit the National Comprehensive Cancer Network, which provides educational resources for patients and families.
Living with Pancreatic Cancer
Living with pancreatic cancer requires balancing treatment demands with emotional and physical well-being. Maintaining open communication with healthcare providers, keeping scheduled follow-up appointments, and seeking second opinions when needed are essential. Patients should not hesitate to discuss pain, nausea, or mental health concerns with their care team; these are integral parts of comprehensive cancer management.
Strong emotional support, nutritional planning, and access to new therapies give patients the tools to face this condition with resilience. Learning more about pancreatic cancer, understanding its risk factors, and knowing what foods to avoid all contribute to better overall care and quality of life.